 On December 7th, the Manicaland Centre organised a satellite session in collaboration with esteemed partners, including the Ministry of Health and Child Care, UNAIDS, the National AIDS Council, Imperial College London, and the South to South Learning Network. This collaborative effort aimed to share our experiences as a country in developing and testing a novel ‘Harare’ HIV Combination Prevention Cascade for use in high-level monitoring and advocacy for the activities and resources needed to strengthen HIV prevention programmes.  Dr Mugurungi, in his introductory remarks, set the stage for the session, followed by insightful presentations by Mr Taramusi from UNAIDS, Dr Moyo from the Ministry of Health and Child Care, and Prof Gregson from the Manicaland Centre for Public Health Research/Biomedical Research and Training Institute. The presentation was followed by a panel discussion where panel members advocated the use of the cascade within national population surveys across the region, emphasising its potential role, similar to the treatment cascade, in driving progress toward UNAIDS targets. The distinguished panel included Mr Mpofu from the National Aids Council, Mr Xaba and Mr Sithole from the Ministry of Health and Child Care, Dr Moorhouse from Imperial College London and Mr Kahn from the South to South Learning Network. The session was a great success. This session was funded by the Bill and Melinda Gates Foundation.
0 Comments
 From December 4th to December 9th, the Manicaland Centre for Public Health Research was well represented at the International Conference on AIDS and STIs in Africa in Harare. Throughout the event, a delegation of representatives from the Centre actively participated and contributed to the vibrant discussions and knowledge exchange. Rufurwokuda Maswera was invited to present one of our studies in an abstract-driven session within the plenary room. His presentation focused on the associations between masculine social norms, sexual risk behaviour and the use of HIV prevention methods in Manicaland. For those interested, a video of his presentation can be found below.  On December 6th, our team members Phyllis Mandizvidza and Blessing Tsenesa made impactful contributions during the poster-driven session. Mrs Mandizvidza shared insights on a study regarding survey measurements of community norms on Adolescent Girls and Young Women’s (AGYW) sexual behaviour and use of condoms for HIV prevention. Mr Tsenesa presented a study on HIV stigma, challenging its potential hindrance to the use of male condoms. Despite persistent high levels of stigma, the study findings suggest that it may not be a barrier to condom use. The Manicaland Centre for Public Health Research recently hosted two workshops in Zimbabwe for national and local stakeholders in the HIV response. The aim of the workshops was to share the results of research by the Manicaland Centre and discuss their policy and programme implications.
Dr Constance Nyamukapa, Research Operations Director of the Manicaland Centre for Public Health Research, has been recognised with a “Highly Commended” award for “Outstanding Achievement through Collaborative Research”. The award was originally presented at the Imperial Faculty of Medicine’s 25th Anniversary Staff Awards in January, but Constance is based in Zimbabwe, so was unable to attend the ceremony. As a result, Prof. Simon Gregson presented the award to Constance at the Manicaland Centre Field Office, in a small gathering on April 4th.
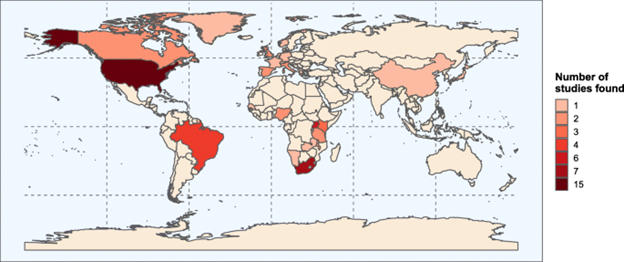
In a short speech, Simon highlighted Constance’s longstanding commitment to research at the Manicaland Centre, and her key role in ensuring that the Centre’s many partnerships are effective. He acknowledged that Constance has led the field operations for the Manicaland Centre successfully since 1998 and continues to play a pivotal role in research on HIV in Zimbabwe. Upon receiving the award, Constance thanked the field team for their support in all the Centre’s research to understand both the HIV epidemic and potential interventions to control its spread. She remarked that she considers her award as recognition of the team’s collective dedication to working together to produce high quality findings. Everyone at the Manicaland Centre congratulates Constance on this remarkable achievement and looks forward to her continued contributions to research at the Centre. High blood pressure is more common among people living with HIV than HIV-negative people in North America, but the reverse is true in Africa and Asia, according to a review of the evidence led by Manicaland Centre researchers. In this post, Manicaland Centre postgraduate researcher Katherine Davis explains the findings. High blood pressure is among the leading causes of death and disability globally. With improved HIV treatment, people living with HIV are beginning to age and develop chronic conditions, including high blood pressure. Nevertheless, it has been unclear whether people living with HIV are more likely to have high blood pressure than HIV-negative people. To bridge this data gap, we systematically reviewed the results from 59 studies of HIV and high blood pressure in adults. We found that high blood pressure is less common among people living with HIV than HIV-negative people globally. However, there are substantial differences by region. In North America, high blood pressure is more common among people living with HIV than HIV-negative people. By contrast, in Africa and Asia high blood pressure is more common among HIV-negative people than people living with HIV. Lastly, in South America and Europe, there isn’t evidence of a difference between people living with HIV and HIV-negative people. It is interesting to consider why we see these differences between regions. One possible explanation relates to diversity in the amount of time that people are exposed to both HIV and HIV treatment. For example, in North America access to HIV treatment and survival of people living with HIV remains better than in Africa and Asia. This may mean that more people have long term exposure to HIV and HIV treatment in North America, which could increase their risk of high blood pressure. Whatever the explanation for the differences, there are important policy ramifications to our findings. In areas with greater burdens of high blood pressure among people living with HIV, targeted prevention of high blood pressure needs to be scaled up. Promoting healthy diets, exercise, avoidance of tobacco, and reduction of alcohol consumption to people living with HIV could have a large impact. Ensuring that people living with HIV can easily access testing and treatment for high blood pressure through integrated, friendly services will also be key. In regions where the burden of high blood pressure is lower and deaths related to AIDS remain common, boosting access to HIV care must continue to be a priority. However, policymakers should also recognise that if access is successfully increased, the population of people living with HIV will age and it is likely that the burden of high blood pressure among people living with HIV will increase. Acting now to bolster prevention and train community healthcare workers in managing high blood pressure could be useful preparation for this. In addition to consequences for policy, our study also has implications for research. Despite a systematic search, we could only find two studies exploring the link between HIV and high blood pressure in Asia. New studies across a range of Asian countries are needed to give us a clearer picture of the relationship between HIV and high blood pressure in the region. With the evidence available today, it is clear that the burden of high blood pressure in people living with HIV varies by region. Our results emphasise the need for expanded prevention and care for high blood pressure, which is tailored to local contexts. Read the systematic review: Association between HIV infection and hypertension: a global systematic review and meta-analysis of cross-sectional studies. Author Katherine is a postgraduate researcher on the Wellcome Trust PhD Programme in Epidemiology, Evolution and Control of Infectious Diseases at Imperial College London. Her work with the Manicaland Centre focuses on non-communicable diseases and mental health. Email: [email protected] Twitter: @kd_katdavis |
Archives
December 2023
Categories |






 RSS Feed
RSS Feed